Judging People for Getting an Epidural
 While there are many strong opinions about using pain medication in labor, the conversation about epidurals and birth often lacks nuance and context. Many pregnant parents feel like they must choose sides, without being mentored on the way systemic policies and ingrained beliefs influence one’s decision on whether or not to have an unmedicated birth. The hospital system, family stories, and cultural conditioning all coalesce to form a lens through which people see birth, both consciously and subconsciously.
While there are many strong opinions about using pain medication in labor, the conversation about epidurals and birth often lacks nuance and context. Many pregnant parents feel like they must choose sides, without being mentored on the way systemic policies and ingrained beliefs influence one’s decision on whether or not to have an unmedicated birth. The hospital system, family stories, and cultural conditioning all coalesce to form a lens through which people see birth, both consciously and subconsciously.
The Medical System
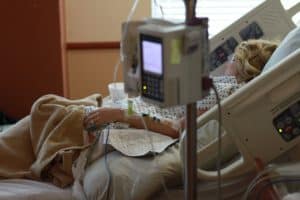
In 2018 I was hospitalized for a couple of days, and found myself shocked at how much of a nuisance my IV was. In my mind I kept saying over and over, “I’m not even having contractions and I want an epidural to deal with how uncomfortable my arm is! How do people labor and birth with an IV?” Two weeks later I still had pain from the nurse trying to insert a new IV in my forearm…the very spot where babies so often rest their heads as they are cradled in their parent’s arms.
The IV is just one piece of apparatus in a collection of technology that modern birthing parents interact with routinely in the hospital system. Two bands around the belly to monitor contractions and baby’s heart rate continuously, an IV, no food or drinks, and remaining in the bed all come on the standard menu.
While there are hospital providers who do intermittent fetal monitoring or use an alternative to the tethered monitors, give Hep Locs (where the IV is inserted but not hooked up to any fluids and the accompanying IV pole unless needed), and encourage drinking, snacking, and freedom of movement; these are exceptions to the norm. Modifying or getting exemptions from common hospital protocols often requires negotiation in the middle of labor (which doesn’t align with the hormonal changes that keep labor flowing), a very specific set of circumstances around the labor, and a hope that the birth attendant who supports more freedom in labor is the one that’s on call that day.
All hospital protocols and interventions have a time and a place where they are very useful. That is the reason why these technologies exist. They can also present emotional and physiological barriers to progress in labor, birth, and infant feeding for low-risk parents.* These practices for birth are, however, well-suited to supporting parents laboring with an epidural.
It’s important to consider the systemic limitations within the spaces where most births occur. We have nurses handling most of the care for laboring parents. Our nurses are assigned so many patients and tasks, that it’s not unusual for them to work through an entire 12-hour shift without enough time to eat, drink, or even use the bathroom. With nurses being stretched so thin, the healthcare system flows better when laboring parents are medicated and able to be monitored from a distance.
Family Stories
While 200 years ago, pregnant people would have witnessed their family members giving birth and nursing babies, modern parents are far removed from the birth scene. Many parents will hold a baby for the first time when they hold their own child. Without exposure to unmedicated birth, parents are left to rely on birth stories from family members and peers who gave birth within the same skewed system, and media images of how to birth and parent. Expectations about birth are implanted into our psyches from early childhood, and become deeply rooted in parents’ impressions of how to give birth. These images almost always show people either laboring with epidurals, or begging for them.
Cultural Conditioning
In the same vein, societal messaging that affects the way parents interact with birth includes stories, sitcoms, and movies with birth scenes. One need only glance at the magazine rack while waiting in line at the supermarket to confirm that people, particularly women, in the West are taught to disconnect from their bodies and their intuition. After years of learning that one’s body is flawed on a constant basis, it can be difficult for parents to suddenly befriend their body and believe in its ability to do the work it needs to do to birth a baby.
![]()
To view the decision to birth with or without epidural medication (or other pain medication) as a single decision existing within one moment of a birth is to ignore the systemic and cultural conditions that are stacked against unmedicated birth. If we’re going to alter the way that birth is allowed to unfold, then it is only fair to alter our attitudes about how parents cope with the intensity of birth. While determination and hard work are an important part of the mindset needed to give birth, compassion and flexibility are equally important. For every condition that makes unmedicated birth less accessible to laboring parents, the wise and compassionate response is to balance it with an equal amount of empathy.
If you are a pregnant parent reading this, I don’t want you to think that your birth is set on a pre-destined path. I do, however, encourage you to explore your ingrained beliefs about birth, parenting, pain, asking for help, and taking up people’s time and attention. When our conditioning is brought to the surface, we have choice where before there was only the ingrained habitual response.
If you are hoping to birth without pain medication, you are well-served to seek out a doctor or midwife who enthusiastically supports that kind of birth, and has plenty of experience in supporting birthing parents through an unmedicated birth. Birth attendants who are tolerant of, or not even tolerant of, the amount of freedom and care that supports an unmedicated birth significantly increase the odds of parents choosing an epidural during the normal (high!) intensity and vulnerability of labor.
No matter your desires for your birth, I encourage you to prepare mindfully for a medicated and unmedicated birth. (The same goes for vaginal and cesarean birth.) Set your compass, create an intention, and be clear on the reasons for your birth preferences. At the same time, resist the temptation to focus all of your preparation on cold, hard facts in lieu of preparing your heart for self-compassion. While we can take actions to influence birth, we cannot control it. Developing compassion for yourself prenatally will help you cope if some of the many factors that determine the direction of a birth change the course of your original plan.
 Nikki Shaheed is the co-owner of Birthing from Within International, and facilitates trainings for birth professionals from around the world. She works with parents prenatally and postpartum in San Antonio, TX, where she lives with her husband and three children. She is also the author of Heart Centered Pregnancy Journal.
Nikki Shaheed is the co-owner of Birthing from Within International, and facilitates trainings for birth professionals from around the world. She works with parents prenatally and postpartum in San Antonio, TX, where she lives with her husband and three children. She is also the author of Heart Centered Pregnancy Journal.
*Continuous monitoring has not been shown to improve outcomes for low-risk birth parents and babies, but rather to cause false alarms that lead to more intervention (link). IV fluids limit laboring people’s mobility and can result in extra difficulties as parents establish a breastfeeding relationship with their newborn baby (link). Not allowing laboring parenting to eat and drink forces a sweeping rule on the masses in an effort to prevent an extremely rare (link) complication of cesarean birth under general anesthesia (link). Those who are able to move or assume an upright position during labor usually find it easier to cope with pain, have shorter labors, and require less medical intervention (link).

Beautifully written, Nikki, and so validating – really takes parents off the hook that they “chose” an epidural. I do see how sometimes parents will opt for an epidural because HOW they are laboring (sounds, movement, etc) makes someone uncomfortable or conflicts with certain hospital and monitoring dogmas.